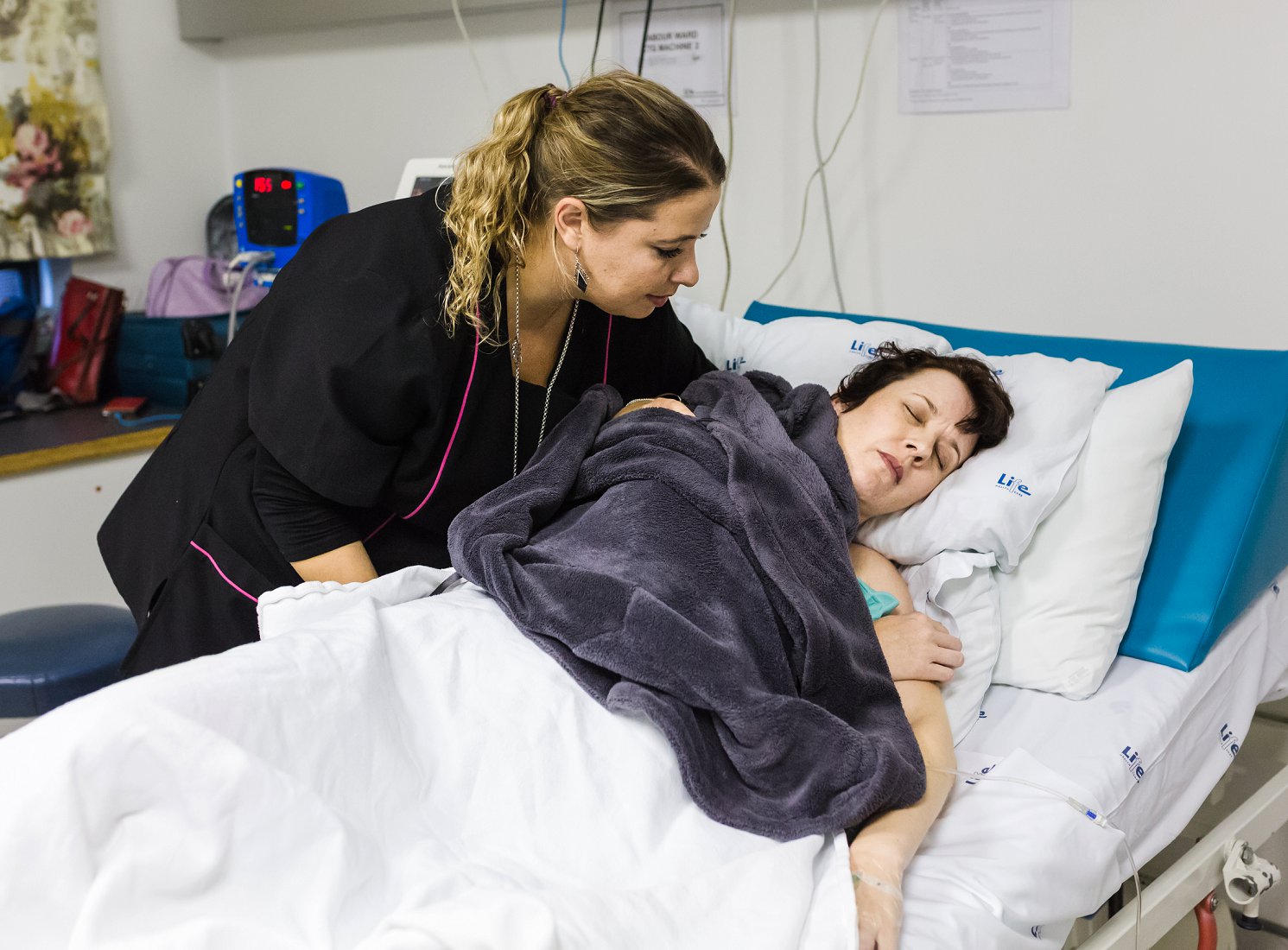
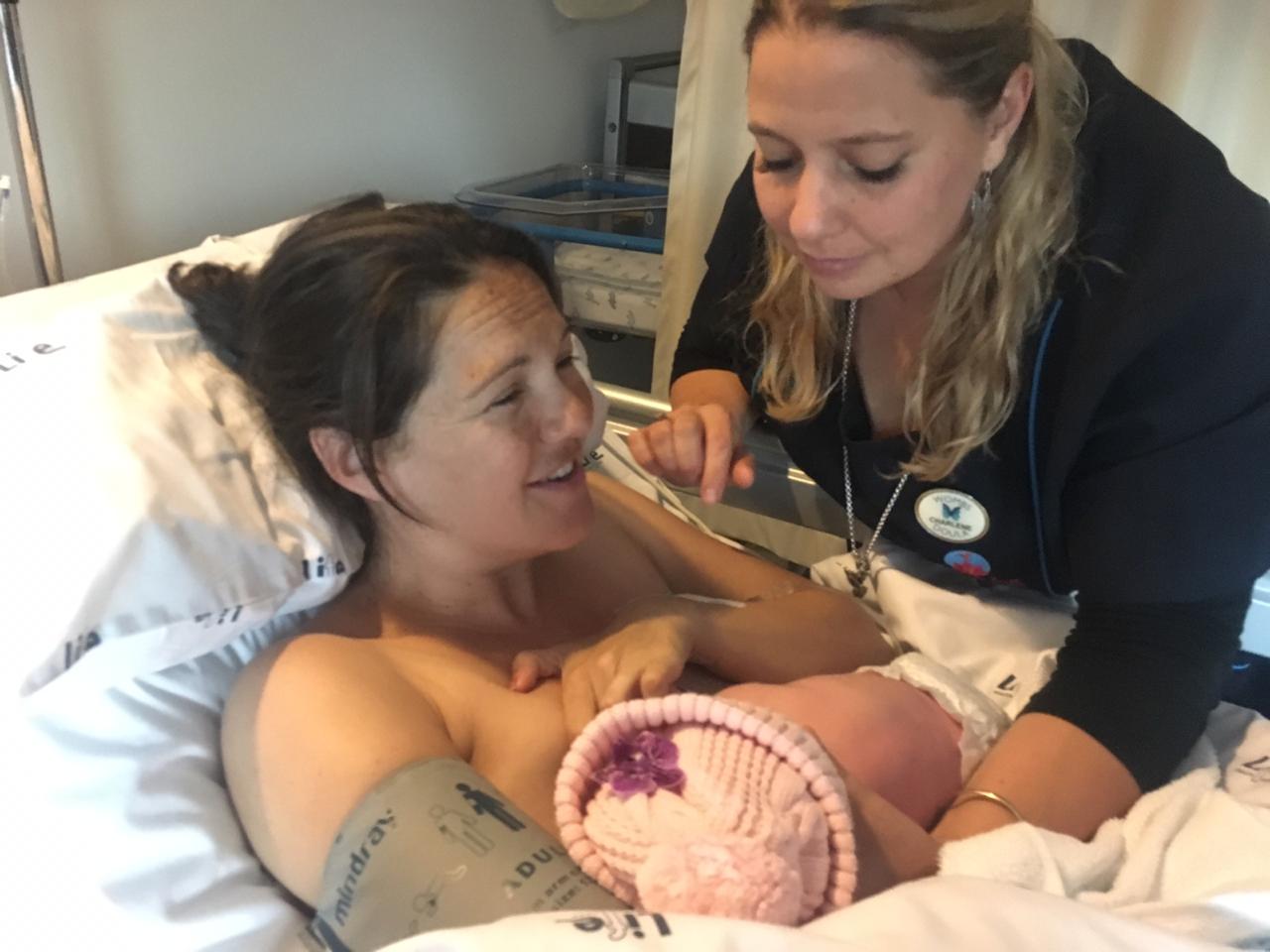
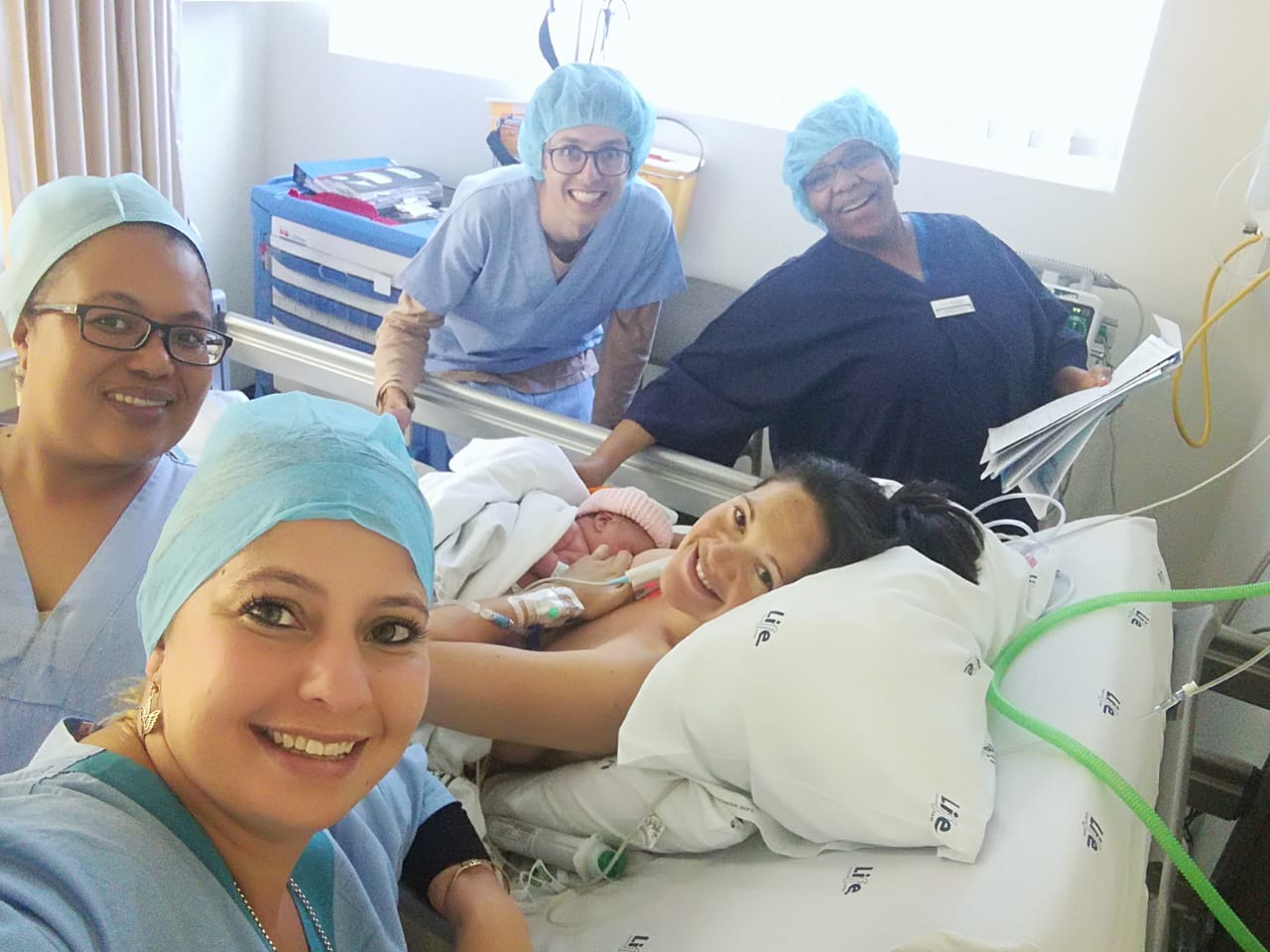
What a pleasure to be Tamlyn’s birth doula. From the moment I met her quite early in her pregnancy, she embodied a certain positivity and exuded a confidence I rarely saw in a first time pregnant mama. She shares her story of trusting the process for her home birth.
I’m a new Mamma, my baby boy Charlie is 4 months old. I’m just starting to emerge from my cocoon of love and bonding, embracing a new way of being and living, finding balance between motherhood and my purpose of serving you. What an incredible journey I’ve been on, from the start of my pregnancy to today, it’s been life changing on so many levels and I am looking forward to sharing it with you.
It all started on the 8th of March at 2.30am when I woke up to a pop, and my waters releasing. I couldn’t believe it was the start of the journey to meet my baby boy. I wanted a natural, intervention free home birth, I was excited and had no idea how things would unfold but had a deep trust that things would happen as they should, a trust and surrendering I’d spent several months cultivating during my pregnancy.
I spent the months leading to my baby’s birth doing the work to birth a new part of myself, a mother. I meditated, visualised, went to healers, coaches and massage therapists, did family constellations work, hypnobirthing, re-created my own birth, did inner child work, went on yoga retreats, painted, walked, prayed and wrote every day. I learned so much. (I have many pregnancy and birth related resources if anyone would like them, please just reply and ask. )
I knew that my pregnancy and birth would have a deep impact on me and my baby and I wanted to go as natural as possible. I had many fears and doubts and whenever they would show up, I would go within and do the work to release them. I’d remind myself to pray for the highest good for all, to let go of control and to remain open to what life would present.
The work for me here was about letting go of the outcome, of control, and also not putting it in the hands of someone else, but to lean in, trust myself, my body, my baby and nature. This was a pattern I’d been playing on repeat most of my life, forever trying to control the outcome of situations or just putting my head in the sand and letting someone else take over. This was my biggest test yet. This time I really wanted to be intentionally conscious of what I wanted to co-create and at the same time know that whatever the outcome, to remain open to what life was offering.
For this reason, I chose my midwives and Charlene Yared-West from Relax Into Birth as my Doula. The moment I met with them, it felt right, very natural and mother and baby-led. I met Charlene at the The Birth Hub Antenatal classes and just loved her segment and felt so comfortable with her. I would highly recommend Charlene as a Doula, I couldn’t have done it without her. Throughout my pregnancy I formed such a beautiful bond with them all and I felt so safe and held with them as my birth team.
So, back to my birth story…
After my waters released, I had very mild intermittent rushes which were not painful at all so I tried to sleep and in the morning I let my midwives know that things could be happening soon. I spent the day painting, watching funny shows and walking in nature to ground myself. I let go of trying to predict what was happening and allowed myself to fold into the experience. I remember thinking to myself, this is easy, I’ve got this. The mild rushes continued on throughout the day and evening and at 10pm that night I told my midwives things were still the same and would get in touch in the morning. As I snuggled up to go to sleep, a strong surge rushed through my body, so strong I had to get on my knees.
A few minutes later, another, I knew it was time. I told Matt to let my midwives and doula that things were progressing. I moved to my birth room where we’d set up the birth pool, affirmations, playlist and positive imagery. I knew now was the time to get out of the way, to let go and let my body and my baby do the work. I instinctively knelt on the floor in the corner of the room on my knees, my upper body resting on my ball. I focused on spiralling my hips and moving back and forth to help the baby move down. The room was dark and quiet and all I could hear was the beautiful kundalini music from my birth playlist which helped me go within.
The surges were coming in heavier and faster now and I was struggling to breathe through them. It was so intense so quickly. (My midwives later told me, I must have had a very good production of Oxytocin as things progressed very quickly in my active labour.) I was beginning to get more and more vocal, my groans and primal sounds getting louder and louder. Matt was sitting with me encouraging me gently, holding my hand which I was using to bear down on with each rush. At about midnight my Doula, Charlene arrived, I was so grateful to see her. By then I didn’t want to speak and was so focused on the surges. She knew exactly what to do to support me. I held her hand she began massaging my lower back which felt so good.
In the meantime, Matt was preparing the birth pool. After a few hours of intense surges, I asked Charlene when she thought I would have my baby, she said soon soon, before the morning which encouraged me. I asked to move into the pool as the rushes were starting to feel unbearable. The moment I slid into the water it was a beautiful relief. It was so warm and took a lot of pressure off my back. However, when the next rush came, I’d forgotten all about the lovely water and roared through the rush. Nature had chosen wild and windy night for my birth which matched exactly what I was going through.
I spent the rest of my labour in the birth pool, on my knees spiralling back and forth while resting my head on the edge of the pool. For each surge I needed to hold someone’s hand, I needed something to push down on, something strong. My doula and Matt stayed by my side for most of my labour alternating for breaks. Giving me water, apple juice and honey to keep up my strength. Charlene let the midwives know when they needed to come and they arrived around 2am, a few hours before my birth. I was hoping they could tell me how close. I asked my midwife, how much longer, and she said ‘’let’s wait and see’’, this was not what I wanted to hear. I wanted her to say any minute now. I had chosen my midwives because they were very trusting in natural birth and in my body to birth my baby, with as little interference as possible however in that moment I wanted answers, my mind wanted to know the outcome, how much longer…! I knew they were doing exactly what they needed to do. I went within and let go.
I had no physical checks during my labour, my midwives spent most of my labour in the other room listening to my labour and doing the occasional listen to my baby’s heart rate which remained steady throughout. My dog Zesa popped into the room a few times wondering what all the noise was about which made me smile to know he was there for me too.
As time went on, I was getting more tired, I really needed him to be close now. My doula Charlene asked Matt what his name was, Matt said we hadn’t decided yet (which we had but he didn’t want to say). She said, if you knew his name you could call him and encourage him out. When I heard that I shouted CHARLIEEEEEE, and they both started laughing, I guess we knew the name after all. I started talking to him, encouraging him, telling him how much he was loved and wanted and that it wasn’t long now. That really helped me. It gave me a new boost of will power and determination. It was like I knew his birth was near. What also helped me was Charlene reminding me to relax and let go of each surge, this really helped me rest in between without tension. She would say one down, one less to go. I could feel he was close now, I muscled up every bit of inner strength I had and focused intently on allowing the birth energy to move through me. I connected with the galaxies and imagined that energy spiralling through me, I knew I didn’t have to do anything, I just need to let go and allow. I looked up at my affirmations and read ‘’I feel the strength of all woman’’. I knew if millions of women had done this before me then so could I. I had no idea who was in the room, and what was happening behind me, I was one with my body and baby.
In my pregnancy I had also done a lot of work listening to Charlene’s Relax into Birth Tracks. In the labour I could hear her voice, saying those calming words over and over again, ‘’relax….open….peace…’’, reminding me to breath ‘’down and out’’.
The next rush brought a new sensation, an excruciating stinging and burning which was incredibly intense. I had read about this in many birth stories but experiencing it was a whole new story. I moaned to Charlene, ‘’IT’S STINGING’’. I remember the song playing at that exact time, ‘’The Power Is Here Now, By Alexia Chellun.
The words to this song were divine timing…
The power of love is here now
The power of now is here now
The power of you and me is here
To create magic on earth
Let the water wash away your tears
Let the fire burn away your fears
Let the wind blow into your life such faith and trust
Let the earth hold you, take care of you and nurture you
This song gave me the strength to get through the final few rushes. I didn’t need to be coached or told what to do. I just listened to my body and my baby. The body truly is built to show you how to birth your baby if you trust it and let it show you the way. Just like in life, you are always being guided, are you listening to that inner guidance.
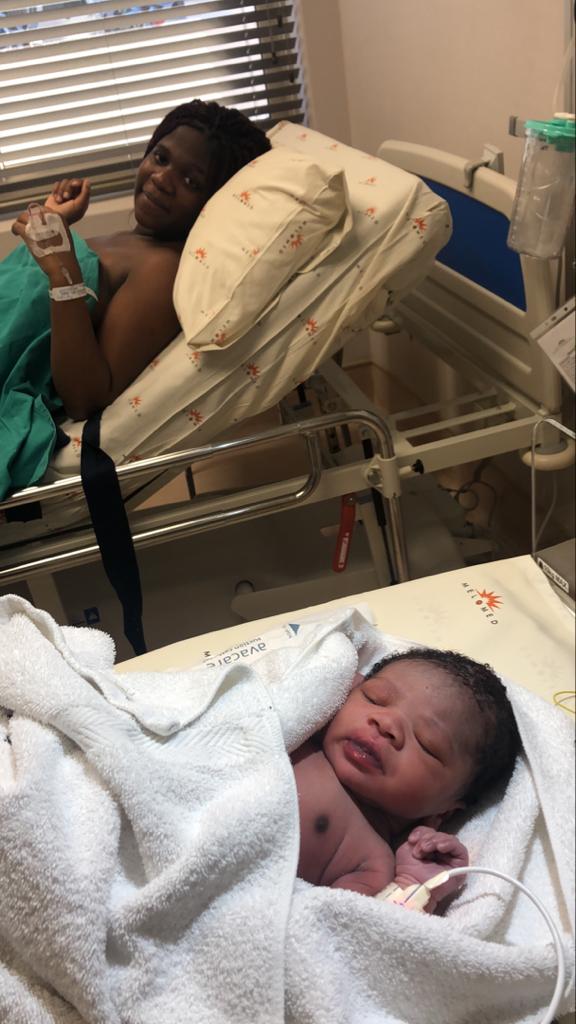
Finally, after an intense surge, and a crazy burning and stinging sensations, my baby’s head came out, and immediate relief came flooding through me, this was it. I then had to stand up and get out of the birth pool and and gave one almighty push and Charlie was born at 4.25am on Monday 9th March weighing 3.92kgs. He slid out into my midwife’s arms. I remember her saying, hello baby, hello baby and rubbing his chest. Charlie was born to the song, Grace of God by Gurunam Singh. It was a special synchronicity that out of my entire playlist Charlie was born to two of my favourite songs and that they came on in the perfect time when I needed them most.
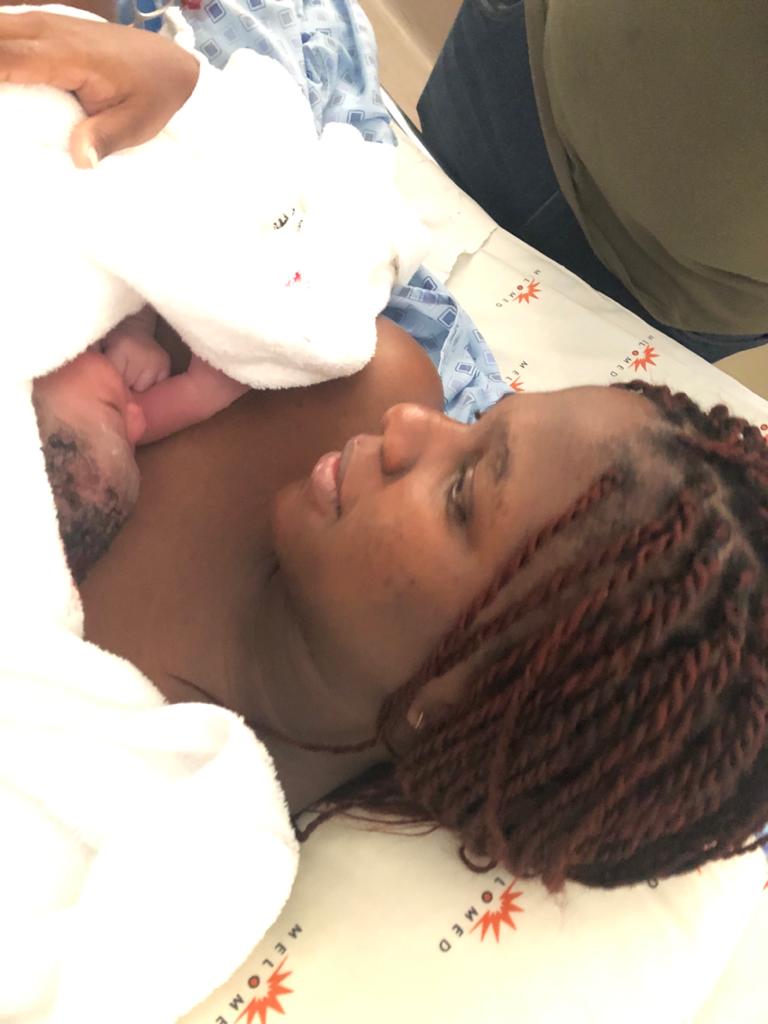
My midwife Lana and Doula Charlene helped me to lay back on the bed and passed my little baby Charlie to me. Matt was by my side through it all. I was completely exhausted and overcome with relief that it was over, and awe that my little man, baby G was finally here. Tears welled in my eyes as held him skin to skin and spoke softly to him. I had done it, we had done it, I had given birth just as I had intended to, at home, naturally, surrounded by love and all was well.
The next few hours were pure bliss. Charlie never left my chest and Matt and I cuddled up in bed and just gazed at him and studied his tiny body. My midwives and doula were incredible, they made our morning even more special. They tidied up around us, brought us tea and left us to bond for a few hours until everyone had had some rest. A few hours later my midwives did all his checks while he lay on Matts chest. I cut the cord and saved my placenta to bury one special day. The next few days were just as incredible getting to know this little soul. He was feeding well, sleeping well and I was in good hands with my midwives coming back every day to check up on us. It couldn’t have been a better first week. I felt so grateful to be a mum and was loving every moment of it. Charlene also came back the week after and gave me the most beautiful foot massage, I felt so taken care of.
Although my birth was pretty close to my dream birth. It wasn’t what I expected. I thought I would breath him out in a blissful meditation. It was way more painful and intense than I ever expected. I could see how woman in hospital would end up with interventions and pain medication and I was just grateful that I was at home and none of that was available. It was just me and my baby working together.
My midwives gave me homeopathic remedies including calendula and seaweed to help with the minor stitches. Charlene made me some beautiful bath salts to soak in. It took me a few weeks to get my energy and strength back, but I am grateful I never had any baby blues or any baby problems. While I was tired, I woke up each day feeling sunshine in my heart so happy to see my little baby. He spent the first week in our bedroom and we didn’t leave home for 40 days. We had minimal visitors, (thanks to Covid-19) and spent our days sleeping, relaxing, singing and getting to know each other. I massaged him daily and he got daily skin to skin and sunshine. We bonded deeply with him and both had the best possible start to our new journey together.
Charlie is now 4 months and thriving. He’s happy, calm, sleeps and feeds well, we’ve never had any issues. I’m so grateful he was born just before lock down, I’m grateful for the bubble it gave us. Just Charlie, Matt, my mum and me. My mum was supposed to be here 3 weeks and ended up being here 4 months, which again was divine planning. I don’t think we could have asked for a better start.
I am incredibly grateful to my birth team. My midwives and Lana who joined on the day and my Doula Charlene. I couldn’t have done it without them. The space they held with me throughout my pregnancy, birth and the days and weeks that followed made this the most incredible experience for me. Their encouragement and trusting approach is what gave me the trust and faith to birth my baby and to be the mum I knew I could be.
I am grateful to Matt for being a non-judgemental support through it all. His help doing everything else allowed me to focus on what I needed to do. We were also so lucky that he got to work from home and still is for this first part of Charlie’s life.
I am grateful to my mum for the 4 months of being here throughout lockdown, her early morning time with Charlie helped me catch up on my sleep, her cooking, cleaning and care, really helped us thrive during these first few months.
I am grateful to my baby Charlie, for being the gift of love and grace that he is. Thank you Charlie for choosing us. We love you.
Thank you for reading my birth story and for joining me on this life-changing journey. A new chapter has begun in my life and I look forward to sharing many more lessons and learnings along the way in the hope that they will too inspire you to live your happiest life.